What Are the Key Differences Between Zirconia and PFM in Implant Restorations?
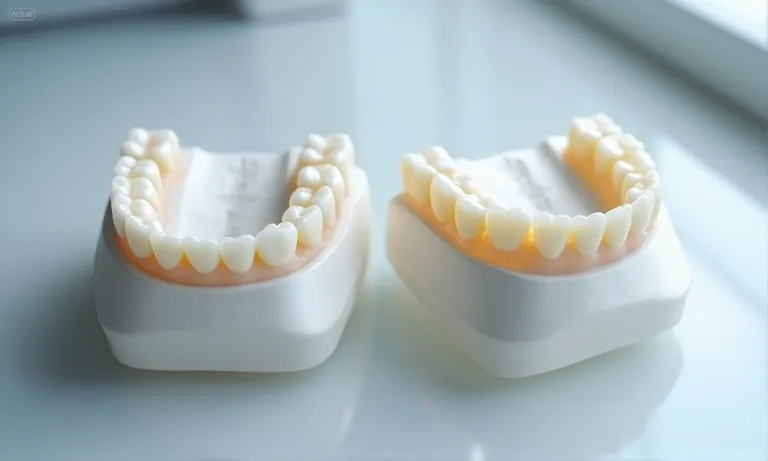
The main differences between zirconia and porcelain-fused-to-metal (PFM) restorations lie in esthetics, strength, and long-term reliability. Zirconia offers lifelike translucency and superior durability, while PFM remains a proven option with metal support but carries esthetic drawbacks such as potential dark gumlines. These distinctions directly affect clinical indications, especially for long-span bridges and full-arch restorations.
Image
ALT: zirconia-vs-pfm-implant-restoration-comparison
Prompt: A highly realistic, ultra-detailed, professional-quality photo captured in a clean, well-lit environment. Materials must be photorealistic, and rendered with DSLR-level clarity. Lighting should be soft daylight or studio white light. Side-by-side display of a zirconia full arch restoration and a PFM bridge on a reflective tray, showing esthetic translucency versus metal-backed structure.
Ready to Partner with You
Let’s Build Your Dental Success Together
Need an expert partner? Connect with our technical team and discover how Raytops can optimize your dental restoration workflow. We’ll contact you within 12 hours with personalized solutions.
12-Hour Response
Expert Consultation
Custom Solutions
How Do Zirconia and PFM Differ in Esthetics and Translucency?
Zirconia restorations provide natural translucency that mimics enamel, making them the preferred choice for anterior or highly visible areas. By contrast, PFM relies on a metal substructure, which can block light and limit esthetic outcomes.
- Zirconia is valued for blending seamlessly with surrounding dentition.
- PFM can appear opaque and sometimes show a visible margin if gum recession occurs.
- For buyers, zirconia is often positioned as a premium option for patients prioritizing esthetics.
Which Material Performs Better in Long-Span Bridges and Full-Arch Cases?
Strength and durability are critical in extended spans. Zirconia has proven high flexural strength, supporting full-arch restorations without significant risk of deformation.
- Zirconia frameworks can handle masticatory forces across full arches.
- PFM provides strong support but may fracture at the porcelain-metal junction under stress.
- For DSOs and larger clinics, zirconia’s reliability in complex cases often justifies its higher cost.
What Are the Risks of Dark Gumline and Long-Term Reliability?
One major drawback of PFM is the potential for dark gumlines over time, particularly if soft tissue recedes. Zirconia, being metal-free, avoids this issue and maintains a more natural esthetic long term.
- PFM: risk of discoloration, higher chance of veneer chipping.
- Zirconia: higher resistance to wear and fewer esthetic failures.
- Both materials can succeed clinically, but zirconia demonstrates better consistency in full-arch applications.
Zirconia and PFM each have a place in implant dentistry, but their differences matter most in terms of case complexity, esthetic demands, and longevity expectations. For buyers, understanding these trade-offs helps align material choice with patient expectations and operational goals. As an overseas dental lab collaborator, Raytops has supported clinics shifting toward zirconia in full-arch cases to balance esthetics and durability in long-term treatment plans.
How Does Material Choice Influence Cost and Long-Term ROI?
Material choice directly impacts both upfront expenses and long-term return on investment (ROI). While zirconia often carries a higher initial price than porcelain-fused-to-metal (PFM), its durability and lower remake rates usually make it more cost-effective over time. Buyers should evaluate not only material costs but also downstream savings tied to efficiency and outsourcing.

implant-restoration-material-cost-roi
How Do Upfront Material Costs Compare with Long-Term Cost-Effectiveness?
Zirconia blocks cost more than PFM components, but ROI must be measured over the restoration’s full service life.
| Factor | Zirconia | PFM |
|---|---|---|
| Upfront Material Cost | Higher per unit | Lower per unit |
| Longevity | 10–15 years typical | 7–10 years typical |
| Risk of Remakes | Lower (3–5%) | Higher (8–12%) |
| Long-Term ROI | Stronger due to fewer replacements | Weaker due to frequent maintenance |
This shows that zirconia’s higher initial investment is offset by fewer failures and better patient satisfaction.
How Do Fewer Remakes and Adjustments Reduce Hidden Expenses?
Hidden costs often appear in the form of remakes, chairside adjustments, or lost clinical time. Choosing zirconia can reduce these issues:
- Less frequent veneer chipping compared with PFM.
- Fewer chairside adjustment appointments for clinicians.
- Reduced lab remake fees and shipping costs.
Over time, even a modest 5% reduction in remake rates can translate into significant annual savings for multi-location DSOs.
What Cost Advantages Come from Bulk Orders and Outsourcing Labs?
Buyers outsourcing zirconia or PFM cases in bulk gain additional savings through economies of scale. Overseas dental labs negotiate material purchases at volume discounts, passing lower per-unit costs to clients. For procurement teams, this improves budgeting accuracy and allows cost control without sacrificing quality.
For example, one distributor noted that outsourcing 200 zirconia frameworks annually reduced their per-unit cost by 15% compared with in-house production. These savings would not have been possible without leveraging lab-scale procurement.
Material choice is therefore not only a clinical decision but also a financial strategy. Buyers working with global dental lab partners like Raytops often see ROI benefits amplified when material advantages combine with outsourcing efficiencies, making zirconia especially attractive for long-term planning.